Bladder Cancer
What is Bladder Cancer?
Bladder cancer occurs when abnormal cells grow and multiply quickly and uncontrollably and invade other tissues.
Bladder cancer can begin in the cells of the bladder lining. In some cases, it may spread into the surrounding bladder muscle. If cancer penetrates this muscle, it can spread to other parts of the body, usually through the bloodstream or lymphatic system.
Bladder cancer is also known as transitional cell carcinoma (TCC) or urothelial carcinoma.
Bladder Cancer’s Health Impact?
If bladder cancer is not caught early, it can spread beyond the bladder and into other body parts, such as the lungs, lymph nodes, and bones. This can make treatment more difficult and decrease the chances of recovery.
In terms of anatomy, bladder cancer may require surgical removal of all or part of the bladder, which can lead to changes in urinary function and bowel function. This can include the need for a permanent urinary diversion, such as an ileal conduit, urostomy or neobladder, which can significantly impact an individual's quality of life.
Bladder cancer can also affect the patient's emotional and mental health. Cancer diagnosis and treatment can be a stressful and emotional experience, and living with the potential side effects of treatment can also be challenging.
How Common is Bladder Cancer?
Bladder cancer is responsible for approximately 3% of all malignancies diagnosed in Australia each year. Bladder cancer is more common in men than women and typically affects people over 60.
Bladder Cancer Causes and Risk Factors
The exact causes of bladder cancer are not fully understood. Still, several factors have been identified that may increase an individual's risk of developing the disease. Some of the most significant risk factors include
- Age: Bladder cancer is more common in older adults, with most cases occurring in individuals over 55.
- Gender: Bladder cancer is more common in men than in women.
- Smoking: Individuals who smoke are at an increased risk of developing bladder cancer, and the risk increases with the number of cigarettes smoked and the length of time the individual has been smoking.
- Exposure to certain chemicals in the workplace, such as those used in the rubber, leather, and chemical industries, may increase an individual's risk of developing bladder cancer.
- Individuals with bladder cancer or a family history of the disease may be at an increased risk of developing it.
- Individuals with chronic bladder inflammation, such as chronic urinary tract infections, interstitial cystitis, or radiation therapy to the pelvis, may be at an increased risk of developing bladder cancer.
- Certain medical conditions, such as Schistosomiasis, a parasitic infection that affects the urinary tract, also increase the risk of bladder cancer.
What are the Symptoms of Bladder Cancer?
The symptoms of bladder cancer can vary depending on the stage and location of cancer. Some of the most common symptoms include
- Blood in the urine (hematuria): This is the most common symptom of bladder cancer and can occur in up to 90% of cases. The blood may be visible or only detectable through a microscope.
- Pain or discomfort during urination (dysuria)
- Frequent urination or urgency
- Lower back pain on one side
- Loss of bladder control
- Inability to urinate
- Pelvic pain
What are the Types of Bladder Cancer?
There are four main types of bladder cancer.
Urothelial Carcinoma (previously Transitional Cell Carcinoma)
Urothelial carcinoma (transitional cell carcinoma) is the most common type of bladder cancer. It begins in the transitional cells in the inner layer of the bladder. Transitional cells change shape without becoming damaged when the tissue is stretched.
Squamous Cell Carcinoma
Squamous cell carcinoma is an uncommon type of bladder cancer in Australia. It begins when thin, flat squamous cells form in the bladder, often after long-term infection or irritation.
Adenocarcinoma
Adenocarcinoma is also rare cancer in Australia. It begins when glandular cells form in the bladder. Glandular cells are what make up the mucus-secreting glands in the body.
These cancer cells have much in common with gland-forming cells of gastrointestinal cancers. Nearly all adenocarcinomas of the bladder are invasive.
Small Cell Carcinoma
This belongs to the neuroendocrine tumour, as cancer is derived from nerve-like cells called neuroendocrine cells.
It accounts for less than 1% of bladder cancers but often grows and invades quickly. It usually needs to be treated with chemotherapy like that used for small cell carcinoma of the lung.
Bladder Cancer Grading
Bladder cancer tumours can be classified based on how the cancer cells appear when viewed through a microscope. This is known as tumour grading, and Dr Wang will describe bladder cancer as either low-grade or high-grade:
- Low-grade bladder tumour. This tumour has cells closer in appearance and organisation to normal cells (well-differentiated). A low-grade tumour usually grows more slowly and is less likely to invade the bladder's muscular wall than a high-grade tumour.
- High-grade bladder tumour. This type of tumour has abnormal-looking cells that lack any resemblance to normal-appearing tissues (poorly differentiated). A high-grade tumour tends to grow more aggressively than a low-grade tumour and is more likely to spread to the muscular wall of the bladder and other tissues and organs.
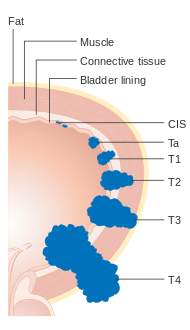
What are the Stages of Bladder Cancer?
The stages of bladder cancer are classified using the TMN staging system.
T (primary tumour) is local staging within the bladder. N (regional lymph nodes) assess whether the tumour has spread to lymph nodes. M (distant metastasis) is positive if the tumour has spread to other organs of the body.
The cancer staging system continues to evolve and is becoming more complex as doctors improve cancer diagnosis and treatment. Dr Wang uses your cancer stage to select the right treatments for you.
If a bladder tumour blocks a ureter (one of the two tubes that pass urine out of the kidneys and into the bladder), patients may experience pain in the side of the body between the ribs and the top of the hip.
In some cases, tumour growth may constrict the urethra (the tube that passes urine from the bladder out of the body) and slow the flow of the urine stream.
Bladder cancers may also shed pieces of dead tissue, fragments of other tissue and other forms of tumour-related matter that are then passed out with the urine.
If the tumour has spread beyond the bladder to surrounding tissue, the patient may experience pelvic pain. In addition, metastases from bladder cancer may cause secondary symptoms, such as bone pain at the site of new cancer.
Bladder cancer that has progressed to the point of organ invasion and metastases may eventually cause the patient to lose weight and feel fatigued. Anaemia and high blood levels of urea and other metabolic by-products, often due to urinary tract obstruction, may be further indications of late-stage bladder cancer.
How is Bladder Cancer Diagnosed?
If blood is in the urine or any other symptoms mentioned are experienced, Dr Wang will need to conduct a clinical assessment and arrange appropriate investigations to formulate an accurate diagnosis.
CT IVP (Intravenous Pyelogram)
CT scans are special x-rays showing your body's internal organs. Dyes may also be injected, allowing the doctor to see the area more clearly if abnormalities are in the upper urinary tract and bladder. CT IVP is the scan investigating upper urinary tract abnormality but requires good kidney function and no contrast allergy.
Renal tract Ultrasound (USS)
Uses sound waves to evaluate the internal genitourinary organs. This test does not require any type of contrast medium. It is indicated when a patient has any contraindication to CT IVP, or the risk of bladder cancer is deemed low (i.e. microscopic haematuria or no risk factors).
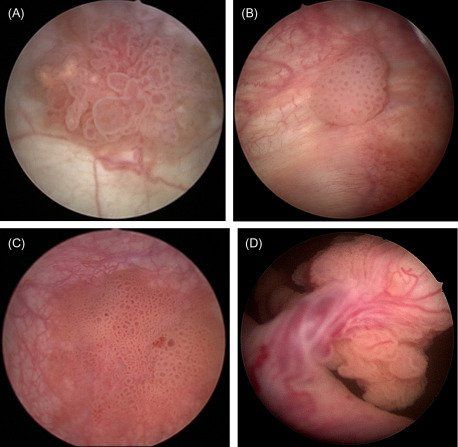
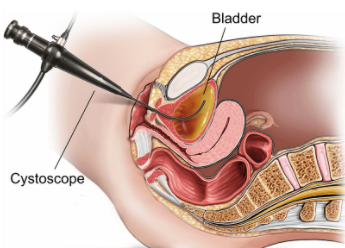
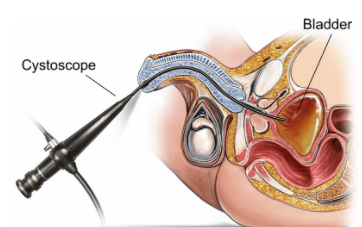
Cystoscopy
Cystoscopy enables a urologist to directly view the inside of the urinary bladder and urethra in great detail using a "cystoscope" (the instrument used). There are two types of cystoscopes.
Rigid Cystoscope
This is a solid straight telescope with a high-intensity magnified light source. A separate channel allows other instruments to be attached.
It will enable urologists to look at the bladder's inner lining and check for abnormalities or suspicious-looking tissue.
Dr Wang may also take a biopsy that can be examined more closely in a laboratory, allowing an accurate diagnosis.
Flexible Cystoscope
This is commonly used for diagnosis and post-op follow-up examinations (e.g. bladder tumour removal). It is a fibre optic instrument that can bend easily and has a manoeuvrable tip that makes it easy to pass along the curves of the urethra.
This procedure may be carried out under general anaesthesia, although many patients tolerate flexible instruments well, allowing this procedure to be done under local anaesthetic on an outpatient basis.
Indications
Dr Wang may perform a cystoscopy to find the cause of many urinary conditions, including:
- Blood in your urine (haematuria)
- Unusual growth, polyp, tumour, or cancer
- Unusual cells found in a urine sample (Atypical/abnormal cytology)
- Frequent urinary tract infections
- Significant lower urinary tract symptoms not responding to behavioural modification or medications
- Loss of bladder control (incontinence) or overactive bladder (Frequent and urgent need to urinate)
- Painful urination, chronic pelvic pain, or interstitial cystitis
- Urinary blockages such as prostate enlargement, stricture, or narrowing of the urinary tract
- Stone in the urinary tract
Urine Cytology
Cells found in the urine are examined under a microscope for abnormalities. This procedure is called urine cytology. This is particularly useful for high-grade (aggressive) bladder or urinary tract cancers. (from the collecting system in the kidney, ureter and bladder)
What are the Treatments for Bladder Cancer?
The choice of treatment depends on several factors, including
- age,
- risk of bladder cancer,
- previous treatment,
- general health and
- the extent and stage of the tumour.
There are several possible treatments available to patients diagnosed with bladder cancer. These include
Non-Surgical Approaches:
Several treatments may be used in conjunction with each other, typical examples being the use of
- Intravesical therapies such as BCG or Chemotherapy (see chemo information),
- Pre-operative (neoadjuvant) chemotherapy or immunotherapy to shrink the tumour or slow its growth in case of muscle-invasive bladder cancer,
- Radiotherapy (in the setting of muscle-invasive bladder cancer in a combination of maximal TURBT and chemotherapy, especially if radical cystectomy is deemed to be risky or patient preference or if symptomatic for palliation)
Surgical Approaches:
- Transurethral Resection of the Bladder Tumour (TURBT)
- Radical Cystectomy
- Urinary Diversion
Dr Wang will discuss with you to ascertain the most appropriate course of treatment for you.
Surgical Treatments for Bladder Cancer
Bladder cancers that have grown into surrounding tissue usually require surgical therapy.
Tumours that have invaded the muscle or tissue around the bladder need surgical management.
Transurethral Resection of the Bladder Tumour
Transurethral Resection of the Bladder Tumour (TURBT) involves inserting a thin tube through the urethra and up into the bladder. The surgeon can then remove the tumour without needing a large external incision.
Radical Cystectomy
A standard form of surgery for muscle-invasive bladder cancer is a Radical Cystectomy, which involves cutting away the entire bladder and associated tissues (including the prostate in men), with Pelvic Lymphadenectomy (removal of the lymph nodes within the hip cavity).
Radical cystectomy in women often includes the removal of the uterus, Fallopian tubes, ovaries, anterior vaginal wall (the front of the birth canal), and urethra. Still, it can be spared to preserve sexual function.
In men, it is also called a Cysto-Prostatectomy, as it involves the removal of the bladder and prostate with Pelvic Lymphadenectomy.
Urinary Diversion
Urinary diversion is a surgical procedure used to redirect the flow of urine when the bladder is removed or cannot function properly. This procedure is sometimes necessary to treat bladder cancer, mainly when the cancer is advanced or has spread to other body parts.
The most common form of urinary diversion is Ileal Conduit. This procedure involves removing the bladder and creating a new passage for urine to flow out of the body. A piece of the small intestine is used to create a new conduit (tube) to carry urine from the kidneys to a stoma (an opening in the abdomen), where a pouching system is worn to collect urine.
This is a major surgery and requires much planning and recuperation time. The suitability of this procedure should be discussed with Dr Wang.
Non-Surgical Treatment for Bladder Cancer
Bladder Cancer treatments include
- Intravesical Treatment
- Radiotherapy for Bladder Cancer
Intravesical Treatment
Intravesical Treatment involves flushing the bladder with chemotherapy or immunotherapy to flush residual tumour cells following surgery. These drugs are placed directly into the bladder to prevent the tumour from recurring or invading the bladder wall's deeper layers.
Researchers have trialled various combinations of systemic medications, and many of these have proven efficacy in the adjuvant treatment of bladder cancers.
Radiotherapy for Bladder Cancer
What is Radiation Therapy?
Radiation therapy, also known as radiotherapy, is a treatment option for bladder cancer that uses high-energy radiation to kill cancer cells. It may be used alone or with other treatments, such as surgery or chemotherapy.
Who gets Radiation Therapy?
Radiation therapy is most commonly used for non-muscle invasive bladder cancer. Still, it may also be used as adjuvant therapy after surgery for muscle-invasive bladder cancer or as a palliative treatment for advanced or metastatic bladder cancer.
Side Effects of Radiation Therapy
Radiation therapy can have side effects, such as fatigue, skin irritation, and urinary problems.
What if Bladder Cancer is Untreated?
Untreated bladder cancer produces significant morbidity, including the following:
- Haematuria
- Dysuria (burning sensation on urination) or Irritative urinary symptoms
- Urinary retention or incontinence
- Upper urinary tract/Ureteric obstruction or kidney failure
- Pelvic or bone pain
- Constitutional symptoms (Fatigue, anorexia, weight loss)
If bladder cancer is not treated and allowed to progress, it can eventually lead to death. Cancer can invade nearby organs, such as the prostate and rectum, and spread to the lymph nodes or distant organs, such as the lungs, liver or bones.
Early detection and prompt treatment are essential for the best outcomes. Regular check-ups and screenings are crucial, especially if you are at higher risk of developing the disease. If you have symptoms or risk factors for bladder cancer, consult your doctor for proper diagnosis and treatment.